Some Roadblocks to Lifesaving Addiction Treatment Are Gone. Now What?
For two decades — as opioid overdose deaths rose steadily — the federal government limited access to buprenorphine, a medication that addiction experts consider the gold standard for treating patients with opioid use disorder. Study after study shows it helps people continue addiction treatment while reducing the risk of overdose and death.
Clinicians who wanted to prescribe the medicine had to complete an eight-hour training. They could treat only a limited number of patients and had to keep special records. They were given a Drug Enforcement Administration registration number starting with X, a designation many doctors say made them a target for drug-enforcement audits.
“Just the process associated with taking care of our patients with a substance use disorder made us feel like, ‘Boy, this is dangerous stuff,'” said Dr. Bobby Mukkamala, who chairs an American Medical Association task force addressing substance use disorder.
“The science doesn’t support that but the rigamarole suggested that.”
That rigamarole is mostly gone. Congress eliminated what became known as the “X-waiver” in legislation President Joe Biden signed late last year. Now begins what some addiction experts are calling a “truth serum moment.”
Were the X-waiver and the burdens that came with it the real reason only about 7% of clinicians in the U.S. were cleared to prescribe buprenorphine? Or were they an excuse that masked hesitation about treating addiction, if not outright disdain for these patients?
There’s great optimism among some leaders in the field that getting rid of the X-waiver will expand access to buprenorphine and reduce overdoses. One study from 2021 shows taking buprenorphine or methadone, another opioid agonist treatment, reduces the mortality risk for people with opioid dependence by 50%. The medication is an opioid that produces much weaker effects than heroin or fentanyl and reduces cravings for those deadlier drugs.
The nation’s drug czar, Dr. Rahul Gupta, said getting rid of the X-waiver would ultimately prevent millions of deaths.
“The impact of this will be felt for years to come,” Gupta said. “It is a true historic change that, frankly, I could only dream of being possible.”
Gupta and others envision obstetricians prescribing buprenorphine to their pregnant patients, infectious disease doctors adding it to their medical toolbox, and lots more patients starting buprenorphine when they come to emergency rooms, primary care clinics, and rehabilitation facilities.
We are “transforming the way we think to make every moment an opportunity to start this treatment and save someone’s life,” said Dr. Sarah Wakeman, the medical director for substance use disorder at Mass General Brigham in Boston.
Wakeman said clinicians she has been contacting for the past decade are finally willing to consider treating patients with buprenorphine. Still, she knows stigma and discrimination could undermine efforts to help those who aren’t being served. In 2021, a national survey showed just 22% of people with opioid use disorder received medications such as buprenorphine and methadone.
The test of whether clinicians will step up and if prescribing will become more widespread is underway in hospitals and clinics across the country as patients struggling with addiction queue up for treatment. A woman named Kim, 65, is among them.
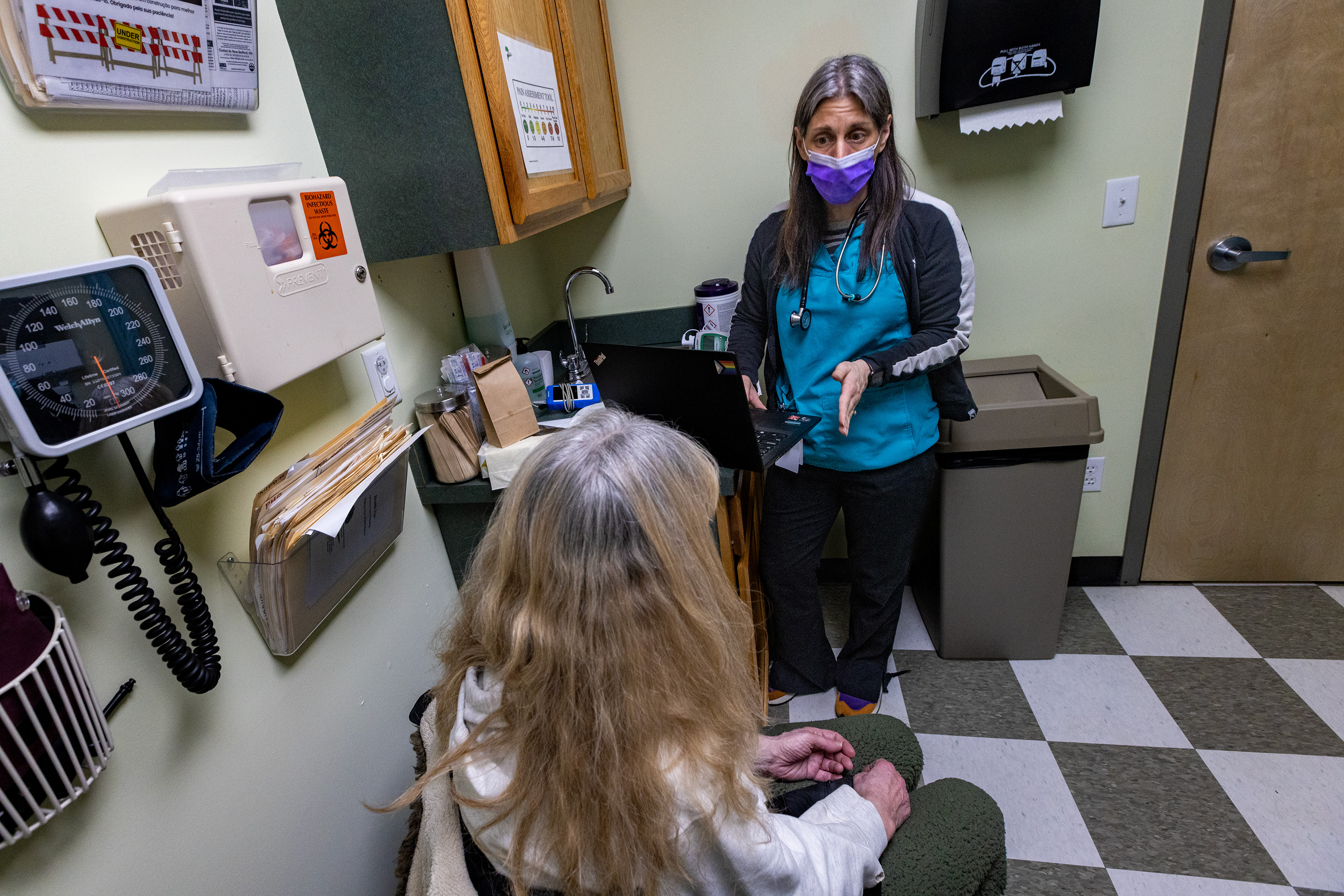
Kim’s recent visit to the Greater New Bedford Community Health Center in southern Massachusetts began in an exam room with Jamie Simmons, a registered nurse who runs the center’s addiction treatment program but doesn’t have prescribing powers. KHN agreed to use only Kim’s first name to limit potential discrimination linked to her drug use.
Kim told Simmons that buprenorphine had helped her stay off heroin and avoid an overdose for nearly 20 years. Kim takes a medication called Suboxone, a combination of buprenorphine and naloxone, which comes in the form of thin, filmlike strips she dissolves under her tongue.
“It’s the best thing they could have ever come out with,” Kim said. “I don’t think I ever even had a desire to use heroin since I’ve been taking them.”
Buprenorphine can produce mild euphoria and slow breathing but there’s a ceiling on the effects. Patients like Kim may develop a tolerance and not experience any effects.
“I don’t get high on Suboxones,” Kim said. “They just keep me normal.”
Still, many clinicians have been hesitant to use buprenorphine — known as a partial opioid agonist — to treat an addiction to more deadly forms of the drug.
Kim’s primary care doctor at the health center never applied for an X-waiver. So for years Kim bounced from one treatment program to another, seeking a prescription. During lapses in her access to buprenorphine, the cravings returned — an especially scary prospect after the powerful opioid fentanyl largely replaced heroin on the streets of Massachusetts, where Kim lives.
“I’ve seen so many people fall out in the last month,” Kim said, using a slang term for overdosing. “That stuff is so strong that within a couple minutes, boom.”
Because fentanyl can kill so quickly, the benefits of taking buprenorphine and other medications to treat opioid use disorder have increased as deaths linked to even stronger types of fentanyl rise.
Buprenorphine is present in a small percentage of overdose deaths nationwide, 2.6%. Of those, 93% involved a mix of one or more other drugs, often benzodiazepines. Fentanyl is in 94% of overdose deaths in Massachusetts.
“Bottom line is, fentanyl kills people, buprenorphine doesn’t,” Simmons said.
That reality added urgency to Kim’s health center visit because Kim took her last Suboxone before arriving; her latest prescription had run out.
Cravings for heroin could have returned in about a day if she didn’t get more Suboxone. Simmons confirmed the dose and told Kim that her primary care doctor might be willing to renew the prescription now that the X-waiver is not required. But Dr. Than Win had some concerns after reviewing Kim’s most recent urine test. It showed traces of cocaine, fentanyl, marijuana, and Xanax, and Win said she was worried about how the street drugs might interact with buprenorphine.
“I don’t want my patients to die from an overdose,” Win said. “But I’m not comfortable with the fentanyl and a lot of narcotics in the system.”
Kim was adamant that she did not intentionally ingest fentanyl, saying it might have been in the cocaine she said her roommate shares occasionally. Kim said she takes the Xanax to sleep. Her drug use presents complications that many primary care doctors don’t have experience managing. Some clinicians are apprehensive about using an opioid to treat an addiction to opioids, despite compelling evidence that doing so can save patients’ lives.
Win was worried about writing her first prescription for Suboxone. But she agreed to help Kim stay on the medication.
“I wanted to start with someone a little bit easier,” Win said. “It’s hard for me; that’s the reality and truth.”
About half of the providers at the Greater New Bedford health center had an X-waiver when it was still required. Attributing some of the resistance to having the waiver to stigma or misunderstanding about addiction, Simmons urged doctors to treat addiction as they would any other disease.
“You wouldn’t not treat a diabetic; you wouldn’t not treat a patient who is hypertensive,” Simmons said. “People can’t control that they formed an addiction to an opiate, alcohol, or a benzo.”
Searching for Solutions to Soften Stigma
Although the restrictions on buprenorphine prescribing are no longer in place, Mukkamala said the perception created by the X-waiver lingers.
“That legacy of elevating this to a level of scrutiny and caution —that needs to be sort of walked back,” Mukkamala said. “That’s going to come from education.”
Mukkamala sees promise in the next generation of doctors, nurse practitioners, and physician assistants coming out of schools that have added addiction training. The AMA and the American Society of Addiction Medicine have online resources for clinicians who want to learn on their own.
Some of these resources may help fulfill a new training requirement for clinicians who prescribe buprenorphine and other controlled narcotics. It will take effect in June. The DEA has not issued details about the training.
But training alone may not shift behavior, as Rhode Island’s experience shows.
The number of Rhode Island practitioners approved to prescribe buprenorphine increased roughly threefold from 2016 to 2022 after the state said physicians in training should obtain an X-waiver. Still, having the option to prescribe buprenorphine “didn’t open the floodgates” for patients in need of treatment, said Dr. Jody Rich, an addiction specialist who teaches at Brown University. From 2016 to 2022, when the number of qualified prescribers increased, the number of patients taking buprenorphine also increased, but by a much smaller percentage.
“It all comes back to stigma,” Rich said.
He said long-standing resistance among some providers to treating addiction is shifting as younger people enter medicine. But tackling the opioid crisis can’t wait for a generational change, he said. To expand buprenorphine access now, states could use pharmacists, partnered with doctors, to help manage the care of more patients with opioid use disorder, Rich’s research shows.
Wakeman, at Mass General Brigham, said it might be time to hold clinicians who don’t provide addiction care accountable through quality measures tied to payments.
“We’re expected to care for patients with diabetes or to care for patients with heart attack in a certain way and the same should be true for patients with an opioid use disorder,” Wakeman said.
One quality measure to track could be how often prescribers start and continue buprenorphine treatment. Wakeman said it would help also if insurers reimbursed clinics for the cost of staff who aren’t traditional clinicians but are critical in addiction care, like recovery coaches and case managers.
Will Ending the X-Waiver Close Racial Gaps?
Wakeman and others are paying especially close attention to whether eliminating the X-waiver helps narrow racial gaps in buprenorphine treatment. The medication is much more commonly prescribed to white patients with private insurance or who can pay cash. But there are also stark differences by race at some health centers where most patients are on Medicaid and would seem to have equal access to the addiction treatment.
At the New Bedford health center, Black patients represent 15% of all patients but only 6% of those taking buprenorphine. For Hispanics, it is 30% to 23%. Most of the health center patients prescribed buprenorphine, 61%, are white, though white patients make up just 36% of patients overall.
Dr. Helena Hansen, who co-authored a book on race in the opioid epidemic, said access to buprenorphine doesn’t guarantee that patients will benefit from it.
“People are not able to stay on a lifesaving medication unless the immense instability in housing, employment, social supports — the very fabric of their communities — is addressed,” Hansen said. “That’s where we fall incredibly short in the United States.”
Hansen said expanding access to buprenorphine has helped reduce overdose deaths dramatically among all drug users in France, including those with low incomes and immigrants. There, patients with opioid use disorder are seen in their communities and offered a wide range of social services.
“Removing the X-waiver,” Hansen said, “is not in itself going to revolutionize the opioid overdose crisis in our country. We would need to do much more.”
This article is part of a partnership that includes WBUR, NPR, and KHN.



