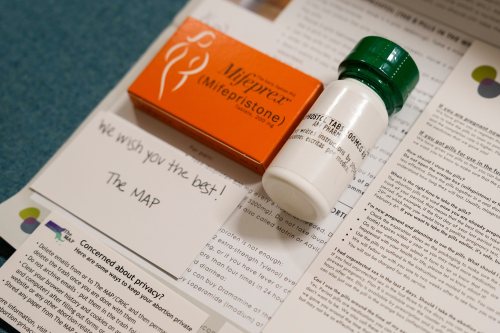
Abortion Pill’s Legal Limbo Continues
The Host

A divided three-judge federal appeals court panel has ruled that a lower court was wrong to try to reverse entirely the FDA’s approval of the abortion drug mifepristone. The panel did find, however, that the agency violated regulatory rules in making the drug more easily available and that those rules should be rolled back. In practice, nothing changes immediately, because the Supreme Court has blocked the lower court’s order that the drug effectively be removed from the U.S. market — for now.
The case is pivotal for the future of reproductive health, as the pill is part of a regimen that is now the most common way American women terminate early pregnancies and is also widely used by doctors to manage miscarriages.
Meanwhile, as President Joe Biden’s Inflation Reduction Act turns one, Medicare officials are preparing to unveil which 10 drugs will be the first to face price negotiation under the new law.
This week’s panelists are Julie Rovner of KFF Health News, Shefali Luthra of The 19th, Sarah Karlin-Smith of the Pink Sheet, and Alice Miranda Ollstein of Politico.
Panelists



Among the takeaways from this week’s episode:
- Wednesday’s federal appeals court decision siding with conservative medical groups challenging mifepristone regulations has perhaps the biggest implications for the drug’s distribution via telemedicine, which has been key to securing abortion access for people in areas where abortion is unavailable.
- The ongoing legal threat to mifepristone is reverberating through the drug industry, as drugmakers worry challenges to the FDA’s scientific authority could cause serious problems for future drug development — especially in an industry that takes big financial risks on getting products approved.
- Texas is suing Planned Parenthood over past Medicaid payments made to the program, charging that the health organization “defrauded” the state, even though the claims were made while a court had specifically allowed Planned Parenthood to remain in the program. Still, the lawsuit emphasizes just how far Texas has gone, and will go, to maintain the legal authority to not support Planned Parenthood, even in its non-abortion work.
- The federal government is expected to release the list of 10 pharmaceuticals subject to Medicare price negotiations by Sept. 1. The drugs’ identities are the subject of much educated speculation, as Congress laid out in the law how drugs qualify for consideration — though even stakeholders in the drug industry are wondering which specific drugs will be up for discussion.
- A national survey of pharmacists finds drug shortages are widespread and leading to rationing at the pharmacy level. A lack of incentives to produce generic drugs is complicating supply-chain problems, leaving fewer options when there are manufacturing or other types of issues with a particular drugmaker.
Email Sign-Up
Subscribe to KFF Health News' free Morning Briefing.
Plus, for “extra credit” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: Time’s “She Wasn’t Able to Get an Abortion. Now She’s a Mom. Soon She’ll Start 7th Grade,” by Charlotte Alter.
Sarah Karlin-Smith: MIT Technology Review’s “Microplastics Are Everywhere. What Does That Mean for Our Immune Systems”? by Jessica Hamzelou.
Shefali Luthra: The Atlantic’s “Right Price, Wrong Politics,” by Annie Lowrey.
Alice Miranda Ollstein: Politico’s “We’re on the Cusp of Another Psychedelic Era. But This Time Washington Is Along for the Ride,” by Erin Schumaker and Katherine Ellen Foley.
Also mentioned in this week’s episode:
- States Newsroom/The Georgia Recorder’s “Study Cited by Texas Judge in Abortion-Pill Case Under Investigation,” by Sofia Resnick.
- Stat’s “From Drug Shortages to High Prices, U.S. System’s Shortcomings Have Deep Roots,” by Matthew Herper.
Click to open the transcript u003cstrongu003eTranscript: Abortion Pill’s Legal Limbo Continuesu003c/strongu003e
KFF Health News’ ‘What the Health?’
Episode Title: Abortion Pill’s Legal Limbo Continues
Episode Number: 310
Published: Aug. 17, 2023
[Editor’s note: This transcript, generated using transcription software, has been edited for style and clarity.]
Julie Rovner: Hello and welcome back to “What the Health?” I’m Julie Rovner, chief Washington correspondent for KFF Health News. And I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Thursday, Aug. 17, at 10 a.m. As always, news happens fast and things might have changed by the time you hear this. So here we go. We are joined today via video conference by Alice Miranda Ollstein of Politico.
Alice Miranda Ollstein: Good morning.
Rovner: Sarah Karlin-Smith of the Pink Sheet.
Sarah Karlin-Smith: Hi, everybody.
Rovner: And Shefali Luthra of The 19th.
Shefali Luthra: Hello.
Rovner: So, no interview this week but plenty of news, particularly for the middle of August, so we will get right to it. The breaking news this week is about abortion and about a Texas abortion case, because 2023. Technically, this news is out of New Orleans, where on Wednesday a three-judge panel of the 5th Circuit federal Court of Appeals upheld, in part, a lower-court decision from Texas that found that the FDA was wrong to approve the abortion pill mifepristone back in the year 2000. Before we get any further in this discussion, we should point out that this decision does not impact the immediate availability of abortion pills. The Supreme Court earlier this spring issued a stay of the lower-court ruling, meaning nothing will change until the full outcome of the case is determined, presumably by the Supreme Court at some point, probably next year. But, Alice, remind us of what this case was about and then what the decision means.
Ollstein: Yeah. So this case is: A coalition of different anti-abortion medical groups that formed last year, specifically formed in the district that a very conservative judge was in charge of down in Texas, brought the case there. And they are going after both the original FDA approval of mifepristone more than two decades ago and a bunch of decisions the agency has made since then to make the pills easier for patients to obtain, like allowing mail delivery, like allowing their use longer into pregnancy than before — 10 weeks versus seven weeks — allowing nonphysicians to prescribe the pills, a bunch of different things.
Rovner: And allowing for a lower dose of the pill actually.
Ollstein: Yes, yes.
Rovner: Which is going to get significant in a second. Go ahead.
Ollstein: Definitely. We should talk about the labeling chaos that could result from this. But so basically, the lower-court judge went all in, agreed with everything they said, essentially, and more or less ordered a national ban. That got stayed. It remains stayed for now, but the 5th Circuit has now weighed in and endorsed some but not all of those arguments. They said, look, the statute of limitations has passed us by on challenging the original FDA approval of the drugs, but they sided with the groups in ordering FDA to get rid of all of those other subsequent decisions. And so this, if upheld by the Supreme Court — we know the Biden administration is already planning to appeal — would really put the pills out of reach for a lot of people. So, it would be a sharp curtailment, but not the total ban the groups were seeking.
Rovner: Yeah, Shefali, and this was obviously what the appeals court had been leaning towards anyway. We know that because that was what they had done before the Supreme Court overruled it. And certainly we know that Justice [Samuel] Alito and I believe Justice [Clarence] Thomas would also do this. So, there’s every reason to believe that this could well be the final outcome. What would it mean? So, the pill would still be approved, but only in the form it was allowed to be distributed before 2016?
Luthra: Precisely, which would be quite significant. You mentioned, right, the need to relabel pills based on the different formulation. We would have pills technically only approved up until seven weeks of pregnancy, although doctors could prescribe them off-label, through 12 weeks in all likelihood. But the telemedicine implications are probably some of the biggest, especially in states where they’ve seen large numbers of out-of-state patients coming for abortion care, right, because they’re near states with bans. Those clinics have really relied on telemedicine because it means they can see more people, and it’s quite safe, right? It’s endorsed by the World Health Organization. You don’t need someone to come in for two, in some cases three visits to get a couple of pills and take them at home. And to lose that would really just cut capacity and make abortions, which are already very difficult to obtain, even in states where it’s legal but there just aren’t as many clinics — like a Kansas, a New Mexico, etc. — if not impossible, very nearly so, just because the math doesn’t work in terms of providers versus patients in need.
Rovner: And the piece of this that I really don’t understand, and I read through the entire decision yesterday afternoon, was they said that the plaintiffs in the case cannot challenge the approval of the generic version of the drug, which was approved in 2019. But of course, the generic version of the drug was approved under the then-rules that that are now going to be rolled back. So you would — would you have a case for the brand name and the generic would have different labeling requirements? It seems very confusing.
Luthra: I think there are a lot of questions that are still open about what this means, right, not only for mifepristone but just for the precedents of FDA approval of medications at large, especially as we’ve seen so many more FDA-approved drugs become more politicized. And, I mean, that’s one of the reasons that so many medical groups have expressed deep concern about this case. It just opens a tremendous can of worms looking well beyond abortion and puts us in pretty uncharted territory for what comes next.
Rovner: And the drug industry is kind of freaked out. Sarah, I guess you could talk to this. I mean, the reliability of FDA approval is now called into question if anybody can basically go to court and say, “Nope, FDA, you shouldn’t have done that,” and possibly win, right?
Karlin-Smith: Right. I mean, they don’t want the scientific sort of authority of the FDA questioned. And I think, you know, like a lot of hot-button political issues where there’s maybe not a good side for them to be on, the pharmaceutical companies tend to try and stay out of abortion politics as much as they can. But some executives and so forth did join amicus briefs in this case because they are concerned about the precedent of FDA approval decisions being able to be challenged in court. And if nothing else, I think drug companies really, and any business to an extent, relies on, like, certainty. And so just having the loss of that certainty that an FDA decision really means, what it means is problematic for them. But I think also these are companies that sort of are based in science and medicine and would definitely prefer to have the assurance that those are the people that approved their drugs and kind of give that seal of approval and it means what it says.
Rovner: Yeah, and the drug industry, I think more than many others, which depends on long shots a lot. I mean, there’s just a lot of dry holes in the drug industry; you spent a lot of time and a lot of money on a drug that ends up not going anywhere. So if you spend a lot of time and a lot of money on a drug that does what it’s supposed to do and gets approved, I think that that could certainly dampen the enthusiasm if then a court could come and say, “Oops, nope.”
Karlin-Smith: And the reputation we talk a lot about, like drug pricing, on this show — the reputation of the FDA and the perceived quality and trustworthiness of its decisions is kind of why the drug companies can charge, to some degree, the prices they charge for their medicines versus, say, you know, we compare it to the supplement industry, which is very loosely regulated, and their claims are not really backed up in the same way by science and medicine. And you can buy those for much cheaper at the store. So their whole business model is really threatened by this.
Rovner: Yeah.
Ollstein: And I think it’s worth noting that one of the three judges on the panel wanted to go further and fully strip FDA approval from the drug, but he was overruled by his other two colleagues. But still, he wrote that dissenting opinion. And that could come into play if and when the Supreme Court takes this up.
Rovner: And he, of course, raised the specter of the Comstock Act, that 1800s-era anti-vice law that apparently some anti-abortion groups are hoping to sort of bring back into the 21st century — Are we in the 22nd century? I’m losing track — and try to figure out if you can just make all of this illegal.
Ollstein: Yes. Judge [James] Ho, who was appointed by [then-President Donald] Trump to the 5th Circuit, and his opinion went a lot further than his colleagues’ in embracing the arguments made by the challengers. So how much influence that has on the process going forward will be really interesting. You know, the Comstock Act has to do with things sent through the mail, and the concern from a lot of legal experts and medical groups is that the interpretation that Judge Ho and these groups are making could mean that sending anything that could potentially be used for an abortion, even if it’s medical equipment that’s also used for other things, could be in jeopardy. And this would be mail delivery. Even sending something to a state where abortion is protected by law could be challenged under this federal rule. And so, we’re definitely in a “throw things at the wall and see what sticks” kind of era. And this is one of the things they’re throwing at the wall.
Rovner: Yeah, just because nothing changes for now doesn’t mean that nothing is going to change. And we will obviously keep a very close eye on this. So last week we talked about a controversy surrounding one of the scientific studies that [District] Judge [Matthew] Kacsmaryk, the lower-court judge, relied on in his ruling. The study was by the Charlotte Lozier Institute. It found that women who had medical abortions were more likely to go to a hospital emergency room within 30 days than women who had surgical procedures. And we talked about how that paper is currently under review by the publisher of the journal the paper appeared in. During the discussion, I apparently misspoke about the paper’s findings, suggesting that it was just the raw number of ER visits that rose along with increased use of medication abortion rather than the rate of the visits. But nonetheless, this study is very much an outlier in three decades of research into the safety of the drug. And I say three decades because it was available in Europe many years before it was available in the United States. And the drug has otherwise been found to have very few serious complications, right?
Luthra: Right. I think you’re absolutely correct, Julie. The study remains an outlier. There remain serious methodological questions about how it came to its findings. And we have an incredibly rich body of research that continues to grow, that shows exactly what you said, which is that the complication rate for medication abortions remains incredibly low. Most people do not require follow-up medical care, especially not in an emergency room. And the reliance on that study in particular was quite striking because of what an outlier it is in the larger medical body of research.
Rovner: And it didn’t actually come up in the appeals court ruling, although they did say, and fair point, they acknowledged that the complication, the serious complication rate, is very low. But if it’s being used by a lot of people and we now know that medication abortion is more than half of all abortions, a very small percentage of a whole lot of people is still a fair number of people. Whether that is enough people to actually create the kind of havoc in emergency rooms that’s been suggested is a different question. But I think that the appeals court justices were fairly careful in the way they worded that. So the mifepristone ruling was not the only news this week about a Texas abortion case. Another Texas abortion case in front of Judge Kacsmaryk in fact: He held a hearing earlier this week in a case brought by the state of Texas to require Planned Parenthood to pay back more than a billion dollars in Medicaid reimbursements, not for abortions, but for family planning and other medical services covered by Medicaid. This one is a weird case even by Texas standards, right?
Ollstein: Yeah, and I’ll say that they’re suing them for more than a billion dollars, but they were only paid by Medicaid in the lower millions. You know, 17-ish million is what Planned Parenthood told me. So, the 1.8 billion is for penalties and damages. They’re accusing them of defrauding the state. So, there has been a many-years’ fight over Planned Parenthood’s participation in Medicaid in Texas specifically, also in other states. Planned Parenthood says that, you know, because lower courts for years blocked the state’s attempt to kick them out of Medicaid, they were perfectly allowed to continue providing nonabortion services, like contraception, tests, whatever, and be reimbursed for that. And the state coming back later and saying that they knowingly defrauded the Medicaid program, they see it as a political attack on them and their ability to keep providing services in the state.
Rovner: There was a court stay on Texas’ desire to kick them out of the Medicaid program, right, so at least at the time it was legal for them to bill Medicaid, and Texas paid the Medicaid claims that they billed, right?
Luthra: I think it’s also helpful to situate this in just a really long history of Texas doing whatever it can to get Planned Parenthood away from government dollars, including turning down millions in federal funding, starting their own state health program for reproductive health, just so that they could have the legal authority to not include Planned Parenthood. This is not really new, but it just is so striking because of the money at stake, because of sort of the tactics, and because of the implications in a world where Planned Parenthood isn’t even providing abortions in Texas anymore.
Rovner: This goes back probably before some of you guys were born, the efforts to sort of defund Planned Parenthood from state and federal dollars, even in states where Planned Parenthood never provided abortions. And there are a number of states where they never provided abortions. But there is a line in the Medicaid statute itself about free choice of providers for patients, and that’s what has been relied on. Lower courts have relied on that for years and years. Congress tried to change it and couldn’t. Texas is actually, I think, the first state that’s ever successfully gotten a court ruling that said they can cut Planned Parenthood out of their Medicaid program. So, it was not odd for Planned Parenthood, while this litigation was going on, to say, “We’re just going to continue to provide women who come to us with family planning and other health care services that we’ve been providing under Medicaid for generations.” But now we’ll see what Judge Kacsmaryk has to say. And then I imagine this will get appealed and we will see where this one ends up, too. Well, finally this week in reproductive health, the American College of Obstetricians and Gynecologists announced the introduction of an online abortion training program, which has been a year in the making, that will give all OB-GYN residents, even in states with abortion bans, access to at least the basics in abortion care and in caring for early pregnancy loss, which is all often the same care. But I have to wonder whether this is going to make students any more willing to do their residencies in states that effectively restrict the rights to practice medicine according to evidence-based standards. I know we’ve talked about this before, but we’re looking at what could be a serious shortage of just women’s reproductive health care in general in abortion ban states, right, if the supply of students wanting to go there to do their residencies and hence stay on afterwards is going to start to dry up?
Ollstein: I mean, it’s already happening for sure. Applications are going down in these ban states. And, you know, when I saw the online curriculum, that’s better than nothing. But all the medical students and residents I’ve spoken to really stress that, in order to be trained and, for some specialties, board-certified, you need practical experience; you need to personally participate in many, many, many abortions to be fully qualified as a physician. And they really stress that the more you do, the more different complications you’re able to observe. And if you only do a few or none and just do online curriculum, you’re not going to be really prepared for a miscarriage situation or any of the many things that could come up in the future. And these could be life-or-death moments. And so to not have people trained and ready to respond in certain states where it’s already hard to recruit people because of, you know, it’s just seen as a less desirable place to be, this is yet another factor. On top of that, you have state attorneys general who have been very litigious and threatening to providers. And so, I’m hearing that that fear is making people not want to practice in particular states.
Luthra: And I think another factor that we don’t often sort of say out loud, but that’s really relevant when it comes to OB-GYNs in training, is that the majority of OB-GYNs are women. And given the age of when people finish medical school, etc., many of them are pursuing residency when they’re at a stage in their life where they might consider getting pregnant, which means that the risks are not just professional or educational; in many cases they are quite personal, and that’s a factor that many people are considering as well.
Rovner: And even the male OB-GYNs in training, many of them are married to women and, again, same age, thinking about, it’s time to start a family. Also, it’s not just the residents themselves, but the residents’ families. I’ve seen that sort of from both sides. We should point out, I mean, there are training programs now and they’re obviously — you know, it’s only been a year, so it’s hard to sort of create these things out of whole cloth — but where residents can travel to other states to get some hands-on experience and training that they want. But again, one of the things we forget sometimes about residents is they don’t earn a lot of money and it’s a disruption. I mean, it’s hard enough to move to a place to do your residency; to then have to sort of pick up and move someplace else for a couple of months to do a rotation is not terribly convenient either. So this is obviously still all being sorted out. But the education of sort of the next generation of reproductive health providers is definitely under question here, right?
Ollstein: And it’s not just the time needed; it’s often the money, because if these people are doing their residency at a public university hospital in a ban state, that public university hospital, under the state law, is afraid to give any money to support them going to another state for training. And so often people either have to apply for grants from foundations to cover that expense or even pay out of their own pockets. So, it’s a real heavy lift.
Rovner: It is. Well, in other news, and there is other news this week, President [Joe] Biden is taking a victory lap as the Inflation Reduction Act, that omnibus health-slash-energy-slash-tax bill, turns 1. But the fate of the highest-profile health policy in that law, calling for Medicare to negotiate the prices of some very expensive drugs, is still in some doubt, as drugmakers sue to try to block the program. Sarah, where is this, and when do we expect to get that list of the first 10 drugs the government wants to negotiate the price of? That’s due soon, right?
Karlin-Smith: Right. So the list is due by Sept. 1 at the latest. So that is a week, I think, from this Friday, or no, a little bit longer than that. But the expectation, I think, is we may get it before Sept. 1, because that’s the Friday before Labor Day weekend.
Rovner: Oh, I don’t know. They love to drop stuff the Friday before Labor Day.
Karlin-Smith: Sometimes they do, and sometimes they also want to take a break too. So, we’re expecting that list of 10 drugs, which would be — their negotiated prices would go into effect in 2026. There’s lots of reasonably well-educated guesses of what those drugs are, because the law sort of lays out how they select them and we have a general sense of how much money is spent on certain drugs in the U.S. and so forth. But Medicare has the most up-to-date data. So, there are still companies that kind of have a sense of, “Oh, I might be on the edge,” depending on how their sales have been in Medicare the past few years. So, people are really curious.
Rovner: Coincidentally or not so coincidentally, I’ve seen some of the speculation, and it is all of the drugs that you see all of those ads for, if you watch, if you still watch, you know, commercial television, on the news or on cable TV. I mean, there are so many ads, and it’s like, surprise, these are all the drugs that are on the likely list that Medicare is going to want to do something about the price of. I assume that is not a coincidence. I’m being snide.
Karlin-Smith: I think some of it is, right, to qualify for the list, you have to be in sort of the top spending categories. And part of that means you’re most likely to have to treat large populations of people. So when you get to drugs like that, like anticoagulants — I think there’s a few expected to be up there — blood thinners, some anti-diabetic medicines, trying to think of some of the other examples. These are kind of mass-market drugs that a lot of people, particularly in the Medicare population, need these medicines. Some cancer medicines, anti-inflammatory drugs. So, it’s not particularly surprising that you would see advertisements for them. And in a lot of cases, too, these are drugs that have some amount of brand competition for them. So, there are two newer blood thinners that might be on there. So, you know, that tends to lead to advertisement when there’s competition in a space. Same for the diabetes medicines and the anti-inflammatories; there’s a lot of expensive biologics in that space that compete.
Rovner: Well, when I’m in charge of the FDA, they’re not going to be able to use, like, songs from the ’60s and ’70s anymore, because that just makes me crazy. Well, meanwhile, in something related to this, drug shortages seem to be getting worse. There’s a new survey from the American Society of Health-System Pharmacists that found that 99% of the 1,100 hospital pharmacists that responded said they were currently managing drug shortages, and one-third said those shortages are forcing them to ration, delay, or cancel treatment. And these aren’t minor drugs. They include cancer chemotherapies, anesthesia drugs, other things that can be difficult to get but important when you need them. Sarah, is this a manufacturing problem, or a marketing problem, or both? I mean, why are drug shortages so much worse now? It’s not all supply chain, is it?
Karlin-Smith: There’s some supply chain, and I think there’s still some supply chain issues that started during covid that are still impacting people. There are manufacturing concerns, depending on the company. You know, drug shortages have gotten a lot of attention recently, but really for probably the past decade or so that I’ve been covering the drug industry and following shortages, the reasons have tended to be the same: They tend to be older, sterile, injectable drugs that are harder to make. But yet, because they have gone generic, the prices have gone down so low that players tend to leave. So only a few players stay in the market because of the pricing situation. So then if they have any manufacturing problem, it can very easily lead to a shortage. Generic companies argue that, you know, there’s just not a lot of incentive for them to invest in redundancy or certain even manufacturing capabilities that might help prevent shortages. So, for better or worse, there really hasn’t been a lot of change in the reasons for these shortages over the years; it’s just that they keep happening.
Rovner: Yeah, well, it’s funny. Matthew Herper over at Stat News has kind of a provocative piece about all of this, suggesting, as you say, that the shortages right now are, in large part, due to the incentives to find the cheapest generics, but that this new Medicare negotiation process — which includes a different clock; it will be based on time on the market rather than time under patent — could encourage drugmakers to do the opposite thing, to sit on new drugs until they can test for all possible uses because they don’t want to bring them to market until they think they can make the most money, because that’s going to determine how long before there can be competition. I mean, is this ever really going to work, being a purely capitalist market?
Karlin-Smith: I mean, there are definitely people, you know, in the shortage space that have argued that some of the current shortages make a good case for public manufacturing of drugs. And actually, it might surprise some people, but the U.S. has engaged in the past in public manufacturing. There are some efforts going on now, like in California; they’re looking into some public manufacturing. So that’s on the generic side. On some of the other situations that Matthew Herper is describing with the IRA, it’s a bit more complicated because essentially the IRA does give companies some amount of time on the market without negotiation. But a lot of drugs, they have all these multiple indications. And so companies are just trying to figure out potentially how they can game their products to make the most amount of money before they’re subject to negotiation. And I know Medicare is quite aware of some of this stuff and is thinking about how they can set up their regulations to protect against that. But not everything is within their control. So we’ll see what happens, because there is concern, you know, particularly I think in the orphan or rare disease space, that a company may delay getting a rare disease indication based on when they think they might get subject to drug negotiations.
Rovner: Every time you think, Oh, they can just lower the price of drugs, it’s super, super complicated. All right. Well, finally this week, there’s something I’ve been trying to get to for a couple of weeks: Before Congress left for the August recess, it passed, on a bipartisan vote, a bill that could finally dethrone UNOS, the United Network for Organ Sharing. UNOS has been the outside organization handling the collection and distribution of human organs for transplant since the federal government began the federal transplant program in 1984. Over the years, UNOS has been roundly criticized for its handling, or mishandling, of the system. But the legislation that originally created the federal organ transplant program had been interpreted not to allow anyone else to compete for the contract to run the network. So, this legislation changes that, for the first time letting other entities see if they can do a better job so maybe fewer people will die waiting for transplanted organs. This feels a lot more important than the attention that it got, I think because there was so much else happening as Congress was leaving town. Or does it feel important to me because I spent so many years and so many hours watching Congress fight over this?
Karlin-Smith: I think it is important. There’s certainly been a lot of big exposés of problems in the system over the years. And there’s also been a lot of, when I’ve covered this more closely in the past, like, tensions between different parts of the country in sort of figuring out how organs are allocated and which parts of regions get impacted or not. So there has always been, like, political dynamics here. I think the underlying thing to watch with this overhaul is that part of what goes on here is we just don’t have enough organs for the number of people that need it. So, you can certainly make improvements and make sure that all the organs we have get to people and get done in the fairest way possible, because there have been lots of concerns around equity issues, particularly that Black people and other people of different ethnicities have not been, you know, getting the organs they deserve. But the question becomes, you know, can anybody do anything about a shortage of organs, and how do you really handle that? I think there’s always going to be tensions on this topic if you don’t have enough organs.
Rovner: Yeah, these were the ultimate formula fights, if you will. You know, it’s usually over money. In the ’90s and early 2000s, it was literally over organs, over, you know, how far you could ship donated organs and whether the large transplant centers should keep more because they do more organ transplants and therefore are more likely to have success. And boy, this fight has been going on for a very long time, but this is at least a step, I think, towards resolving it. All right. Well, that is this week’s news. We will take a quick break and then we will come back and do our extra credit. Hey, “What the Health?” listeners, you already know that few things in health care are ever simple. So, if you like our show, I recommend you also listen to “Tradeoffs,” a podcast that goes even deeper into our costly, complicated, and often counterintuitive health care system, hosted by longtime health care journalist and friend Dan Gorenstein. “Tradeoffs” digs into the evidence and research data behind health care policies and tells the stories of real people impacted by decisions made in C-suites, doctor’s offices, and even Congress. You can subscribe to “Tradeoffs” wherever you get your podcasts. OK, we are back and it’s time for our extra credit segment. That’s when we each recommend a story we read this week we think you should read too. As always, don’t worry if you miss it; we will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Shefali, why don’t you go first this week?
Luthra: My piece is from The Atlantic, by Annie Lowrey. The headline is “Right Price, Wrong Politics.” It is incredibly smart. It is about how there is all this conversation about people wanting to move to states where they have access to health care protected, whether that is abortion or gender-affirming care, etc., etc. There is one problem, which is that those states are largely ones where it is much more expensive to live, because of housing prices. And if you want to live in a place where you can afford a home, those are often the states with restrictions on health care. I love this piece. I think there is so much conversation about, Why don’t people simply move to a place where state laws reflect what they would like? And the answer is it’s really not attainable for most people. And I think she does a great job of explaining why that is and putting it in the context of policy choices and not just sort of individual human elements.
Rovner: I was super jealous of this piece. It was like, Oh, yeah, of course. Alice.
Ollstein: I chose a piece by a couple of my colleagues, and it’s called “We’re on the Cusp of Another Psychedelic Era. But This Time Washington Is Along for the Ride.” And it’s about how much bipartisan support there is in Congress right now for making psychedelics more available as medicine to treat things like PTSD [post-traumatic stress disorder] or depression. There are just a lot more clinical trials going on right now and just support for making them available through the VA [Department of Veterans Affairs] as sort of a test of how a broader population might respond. You know, we’re talking about things like psilocybin, things like ketamine, things like ecstasy, that have shown a lot of promise in having a therapeutic benefit for mental health conditions that have resisted other forms of treatment. So, fascinating stuff.
Rovner: It is. Sarah.
Karlin-Smith: I took a look at a piece in MIT Tech Review called “Microplastics Are Everywhere. What Does That Mean for Our Immune Systems?” And it just does a good job of helping you understand what the research has shown about how these very tiny particles may impact your immune cells and then impact our ability to fight off diseases and maybe even lead to more challenges with antibiotics and antibiotic resistance. And I’ve been fascinated by all the coverage of this, because this — huge problem and, you know, they talk about them being in our air and in the deepest part of the ocean. And, you know, it’s just one of those things that we have to kind of grapple with as a society, like health, economic consequences, and so forth. So, it’s worth looking at.
Rovner: More things to keep us awake at night.
Karlin-Smith: Exactly.
Karlin-Smith: A list of more things to keep us awake at night. My story this week is one of the most talked about on social media. It’s from Time, and it’s called “She Wasn’t Able to Get an Abortion. Now She’s a Mom. Soon She’ll Start 7th Grade,” by Charlotte Alter. And as the headline indicates, it’s kind of a gutting piece about a 12-year-old in Mississippi who was raped in her own yard, was too scared to tell anyone, and ended up having a baby at age 13. It’s another story about all those things that are, quote, “made up,” or not supposed to happen. Except they did. She might have been eligible for a rape exception, except there are no abortion providers left in the state, and her mother didn’t know that rape exceptions were a possibility. In the end, the closest place for her to have gotten an abortion was Chicago, which was too far and too expensive for her family. So now she has a son while she’s going to middle school. I’m sure we will see more of these as time progresses. All right. That is our show for this week. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review; that helps other people find us too. Special thanks, as always, to our amazing engineer, Francis Ying. And as always, you can email us your comments or questions. We’re at whatthehealth@kff.org. Or you can tweet me or X me or whatever. I’m still there, @jrovner, also on Bluesky and Threads. Shefali?
Luthra: I’m @shefalil.
Rovner: Alice.
Ollstein: @AliceOllstein.
Rovner: Sarah.
Karlin-Smith: I’m @SarahKarlin or @sarahkarlin-smith.
Rovner: We will be back in your feed next week. Until then, be healthy.
Credits
To hear all our podcasts, click here.
And subscribe to KFF Health News’ ‘What the Health?’ on Spotify, Apple Podcasts, Pocket Casts, or wherever you listen to podcasts.