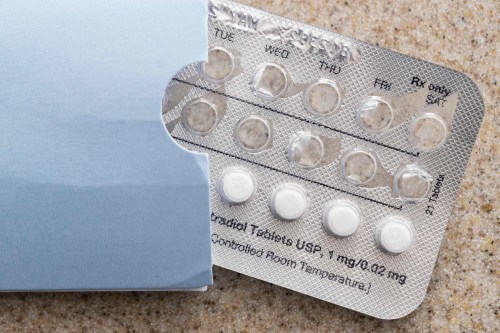
New Guidelines May Drop Birth Control Training Rule
This story comes from our partner

‘s Shots blog.
One of the more popular provisions of the federal health law requires that women be given much freer access to prescription methods of birth control. That includes not only the pill, but implants and IUDs as well.
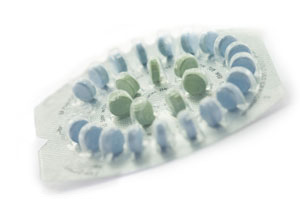
But what happens if there are not enough doctors to prescribe those contraceptives?
That’s exactly what worries some reproductive health advocates, as efforts are underway to rewrite rules governing the training of the nation’s family doctors.
The proposed new rules, they say, drop existing requirements that family medicine residents be required to undergo training in contraception and counseling women with unintended pregnancies. Several groups are now running letter-writing campaigns to make sure the rules remain.
Revising The Rules
Family physicians are what used to be known as general practitioners, or GPs.
“My youngest patient hasn’t been born yet, and the oldest I take care of is 94,” says Jeff Cain, president of the American Academy of Family Physicians and a family doctor in Denver.
For the majority of women, particularly outside major cities, it’s family doctors, not obstetrician-gynecologists, who provide for their reproductive health needs.
“The main people who staff community health centers, as well as large swaths of rural America, are family doctors,” says Linda Prine, a family physician from New York.
To become a family doctor, however, medical residents must complete a wide-ranging and rigorous three-year training program approved by the Accreditation Council on Graduate Medical Education.
Every seven years, the ACGME guidelines for each specialty are revised; it’s now time for a rewrite of the family medicine curriculum.
Prine, who is also the medical director of the Reproductive Health Access Project, helped lead a push the last time around to require all family medicine residents to learn to provide all forms of prescription contraceptives, including placing IUDs and implants, and to counsel patients with unintended pregnancies on their options.
“The language was put in so that we would be assured that family doctors were prepared to provide health care for their patients,” she says.
But now that requirement appears to be going away.
“The feedback we’ve gotten over the years is that a lot of the curricular requirements were too specific,” says Peter Carek, a professor of family medicine at the Medical University of South Carolina and chairman of the committee that’s rewriting the requirements for family medicine residents.
“So in general what we’ve tried to do as a committee is to at least in as many areas as we could, pull back some of those specific requirements and give them more general requirements to follow,” he says.
Criticism
Reproductive health advocates say there’s a big problem with leaving contraception training up to each program: Many residency programs these days are run by religious hospitals that don’t believe in contraception.
“The way it works right now, the residency is required to at least send the residents off-site to another place, say, a family planning clinic where they can learn how to provide birth control,” Prine says. “If these regulations change and there’s no wording whatsoever about the need to provide contraception, the residency programs would no longer be obliged to send their residents somewhere where they would get this education.”
If you think that religious-based health care isn’t becoming the norm, think again.
“We took a look recently and found that of the 25 largest health systems in the United States, 13 were religiously sponsored; that includes 11 Catholic systems,” says Lois Uttley, who heads the nonprofit group MergerWatch, which works to protect women’s access to reproductive health care when secular hospitals merge with religious ones. “So that means the likelihood of a patient encountering a Catholic restriction on contraception is pretty high and growing.”
Draft Document
Family medicine officials, however, say they are aware of the concerns from reproductive health advocates.
“The American Academy of Family Physicians and family medicine educators really remain committed to ensuring that women’s health is a core educational part of training family physicians,” says Cain, the AAFP president. “That includes family planning and maternity care.”
Cain says that while the new program standards may not spell out the contraceptive training requirements the way the current ones do, he expects they will be included in a frequently asked questions part of the document that will still carry the same weight.
In any case, he points out, “the truth is this is a draft document right now. We want to make sure the wording in the document reflects the intended outcome.”
Both Cain and Carek say they are taking under serious consideration all the comments they have been hearing about the standards so far.
The last day for the public to comment is Thursday.