The Policy, and Politics, of Medicare Advantage
The Host

Medicare Advantage, the private-sector alternative to original Medicare, now enrolls nearly half of all Medicare beneficiaries. But it remains controversial because — while most of its subscribers like the extra benefits many plans provide — the program frequently costs the federal government more than if those seniors remained in the fully public program. That controversy is becoming political, as the Biden administration tries to rein in some of those payments without being accused of “cutting” Medicare.
Meanwhile, President Joe Biden has signed a bill to declassify U.S. intelligence about the possible origin of covid-19 in China. And new evidence has emerged potentially linking the virus to raccoon dogs at an animal market in Wuhan, where the virus reportedly first took hold.
This week’s panelists are Julie Rovner of KHN, Margot Sanger-Katz of The New York Times, Jessie Hellmann of CQ Roll Call, and Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico.
Panelists



Among the takeaways from this week’s episode:
- The Biden administration recently changed the formula used to calculate how much the federal government pays private Medicare Advantage plans to care for patients with serious conditions, amid allegations that many of the health plans overcharge or even defraud the government. Major insurers are making no secret about how lucrative the program can be: Humana recently said it would leave the commercial insurance market and focus on government-funded programs, like its booming Medicare Advantage plans.
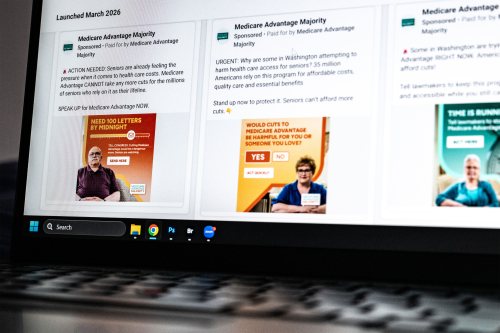
- The formula change is intended to rein in excess spending on Medicare — a huge, costly program at risk of insolvency — yet it has triggered a lobbying blitz, including a vigorous letter-writing campaign in support of the popular Medicare Advantage program. On Capitol Hill, though, party leaders have not stepped up to defend private insurers as aggressively as they have in the past. But the 2024 campaign season could hear the parties trading accusations over whether Biden cut Medicare or, conversely, protected it.
- The latest maternal mortality rates released by the Centers for Disease Control and Prevention show the problem continued to worsen during the pandemic. Many states have extended Medicaid coverage for a full year after women give birth, in an effort to improve care during that higher-risk period. But other problems limit access to postpartum care. During the pandemic, some women did not get prenatal care. And after the fall of Roe v. Wade, some states are having trouble securing providers — including one rural Idaho hospital, which announced it will stop delivering babies.
- The federal government will soon declassify intelligence related to the origins of the covid pandemic. In the United States, the fight over what started the pandemic has largely morphed into an issue of political identity, with Republicans favoring the notion that a Chinese lab leak started the global health crisis that killed millions, while Democrats are more likely to believe it was animal transmission tied to a wet market.
- And in drug price news, Sanofi has become the third major insulin maker (of three) to announce it will reduce the price on some of its insulin products ahead of a U.S. government policy change next year that could have cost the company.
Email Sign-Up
Subscribe to KFF Health News' free Morning Briefing.
Plus, for “extra credit,” the panelists suggest health policy stories they read this week that they think you should read, too:
Julie Rovner: Vice News’ “Inside the Private Group Where Parents Give Ivermectin to Kids With Autism,” by David Gilbert
Jessie Hellmann: The Washington Post’s “Senior Care Is Crushingly Expensive. Boomers Aren’t Ready,” by Christopher Rowland
Joanne Kenen: The New Yorker’s “Will the Ozempic Era Change How We Think About Being Fat and Being Thin?” by Jia Tolentino
Margot Sanger-Katz: Slate’s “You Know What? I’m Not Doing This Anymore,” by Sophie Novack
Also mentioned on this week’s podcast:
- Coverage by KHN’s Fred Schulte on Medicare Advantage: https://kffhealthnews.org/news/author/fred-schulte/
- The New York Times’ “Biden Plan to Cut Billions in Medicare Fraud Ignites Lobbying Frenzy,” by Reed Abelson and Margot Sanger-Katz
- The CDC’s “Maternal Mortality Rates in the United States, 2021,” by Donna L. Hoyert
Click to open the transcript Transcript: The Policy, and Politics, of Medicare Advantage
KHN’s ‘What the Health?’
Episode Title: The Policy, and Politics, of Medicare Advantage
Episode Number: 290
Published: March 23, 2023
[Editor’s note: This transcript, generated using transcription software, has been edited for style and clarity.]
Julie Rovner: Hello and welcome back to KHN’s “What the Health?” I’m Julie Rovner, chief Washington correspondent at Kaiser Health News. And I’m joined by some of the best and smartest health reporters in Washington. We’re taping this week on Thursday, March 23, at 10:30 a.m. As always, news happens fast, and things might have changed by the time you hear this. So here we go. Today we are joined via video conference by Margot Sanger-Katz of The New York Times.
Margot Sanger-Katz: Good morning, everybody.
Rovner: Jessie Hellmann of CQ Roll Call.
Jessie Hellmann: Hello.
Rovner: And Joanne Kenen of the Johns Hopkins Bloomberg School of Public Health and Politico.
Joanne Kenen: Hi, everybody.
Rovner: So a happy 13th birthday to the Affordable Care Act, which President Obama signed just a couple of hundred feet from where I am sitting now. But there’s lots of other health news, so we’re going to dive right in. I want to start this week with Medicare Advantage, the private Medicare alternative that now enrolls more than half of all Medicare beneficiaries. If you watch cable TV or pretty much any TV at all, you have likely seen the dueling ads. They’re part of a multimillion-dollar lobbying campaign, like this ad from the Better Medicare Alliance, made up of mostly Medicare Advantage insurers.
Excerpt from ad set in a bowling alley:
Bowler 1: They might cut Medicare Advantage.
Bowler 2: C’mon!
Bowler 1: They’re talking about it in Washington.
Bowler 2: Cut Medicare Advantage? Higher premiums? With inflation already so high?
Bowler 3: That’s nuts!
Rovner: Or this one from the consumer advocacy group Protect Our Care.
Excerpt from ad: Insurance companies are lying to America’s seniors about cuts to Medicare Advantage benefits. Experts agree what they are saying is just plain false. Health insurance companies are simply trying to stop cuts to their sky-high profits, CEO salaries, and bonuses.
Rovner: I swear, Margot, I pulled the clip from that first ad before you also used it in your excellent story published Wednesday. So — and I know this is a hugely complicated issue that we’re going to try to take apart at least a little bit — but, who’s right here? Those who are saying that Medicare Advantage is about to be cut or those who were saying not really.
Sanger-Katz: I think actually they are both a little bit right. The Biden administration has made a very technical change to the formula that pays these private plans extra money when they sign up patients who have serious medical diagnoses. And this is, of course, a response to an earlier problem. It used to be Medicare Advantage plans — those are the private plans that are an alternative to the government Medicare program. It used to be that they just got a flat fee for everyone that they signed up. That was about what it costs on average to take care of someone in Medicare. And what happened is that the plans then had a huge incentive to only sign up healthy people. And so that’s what they tried to do. And they marketed to healthy people by doing things like including gym benefits in the health insurance plan or this famous, and perhaps apocryphal, example of, you know, locating the enrollment office on the third story of a building with no elevators so only people who could get up the stairs would be able to sign up for the plan. And so, there was this policy response where it said, well, you know, sicker people are more expensive to take care of, and we want these plans to not just be cherry-picking all of the healthiest people. And so they created this system that basically pays extra to the plans. If you have congestive heart failure, if you have cancer, or if you have diabetes, then your health plan gets, like, a little bonus. But what we have seen over the course of the life of this program is that this has created enormous incentives for the plans to diagnose their customers with as many diseases as possible, regardless of the strength of the evidence that they have. And there is a whole industry of data-mining operations that go through people’s medical records, of home health agencies that go into people’s homes just to diagnose them with more illnesses. And there are just absolutely widespread — from, like, every possible authoritative source that you can think of — allegations of overcharging of the federal government through this program and also of fraud. Not every insurance plan in the country in this program has been accused of fraud, but quite a lot of them have, including most of the largest players. And they are facing lawsuits in federal court for basically scamming Medicare by saying that their people are too sick.
Rovner: So I want to go back to the beginning or, really, the middle. Medicare has offered beneficiaries the option of enrolling in a private managed-care plan instead of what’s known as traditional Medicare, where patients can go to just about any doctor or hospital, pretty much from the inception of the program and pretty broadly since the Reagan administration in the early 1980s. They were originally called Medicare risk plans. Health plans almost exclusively, HMOs, said they could provide the same care more efficiently by, quote, “managing care,” and could still make a profit even if the government paid them 5% less than the average patient in traditional Medicare in that area. So it was a good deal all around. The plans were making money. The government was saving money. Yeah, that was a very long time ago. Since then, Congress has significantly raised what it pays the plans with the stipulation that they use the excess funds to either reduce premiums or add benefits, mostly dental, vision, and hearing care. Still, however, a lot of insurers are, to use a technical term, raking it in. In fact, Humana last month announced that it was going to pull out of the commercial insurance market in order to concentrate on its much more lucrative Medicare Advantage business. So, how are these companies both providing more benefits and making big profits? I know that fraud is part of it. Jessie, where’s all this money coming from?
Hellmann: Like Margot said … I think a lot of it has to do with the upcoding that they do. They’re just able to find all of these diagnoses from their enrollees, either through chart reviews … some have done home health visits where they send in people to interview patients and ask about their health history without really providing any care. So that’s another way. And it’s just become, like, a really lucrative business practice for them. But like Margot said, they’ve just been facing more and more scrutiny and lawsuits over the way that they do this.
Rovner: They deny care, too, right? That has been a long-standing issue that people who go into these plans and then get sick sometimes have trouble getting the care that they need.
Hellmann: Medicare Advantage plans do something called prior authorization, where they require providers submit requests for something to be covered before they’ll pay for it. They do this with a lot of more costly things, like imaging or like nursing home stays, which are obviously very expensive. And so if they can deny these claims and maybe get a beneficiary to do something that is cheaper before moving onto these more costly things, then that obviously saves some money. But that’s something else that the Biden administration has been looking more closely at. They’ve proposed a few rules that would just say that Medicare Advantage plans have to cover things that are covered by Medicare. They can’t just deny care for something based on their own proprietary models of deciding whether something is medically necessary or not.
Kenen: It’s complicated because sometimes there are patients that ask for things that they actually don’t need. You know, something they have seen on TV or they heard their neighbor had or whatever, and that [there’s] actually something more conservative [that can be done]. Back surgery is the famous example. You know, sometimes physical therapy and other treatments will do better than an $80,000 back surgery. But there’s a difference between saying, “Let’s try something else first,” and times when somebody is really sick and needs an expensive drug, they may have already tried a cheaper drug in another health plan the year before. It’s very hard to untangle, you know, when “no” is appropriate because we have overtreatment in this country. But the problem here is that sometimes “no” it’s completely inappropriate, and the insurer is not paying for something that the patient expected to get when they signed up for a health plan to take care of their health.
Rovner: And we should point out this is true in all managed-care plans, not just in Medicare Advantage plans.
Kenen: Yes.
Rovner: So before we move on, I want to give a shoutout to my KHN colleague Fred Schulte, who has been on the Medicare Advantage fraud trail like a dog with a bone for more than a decade now. We will link to some of his award-winning work in our show notes. Anyway, now the Biden administration, Margot, as you said, is trying to crack down on the, if not outright fraud, at least the manipulation of payments, which will also, at the same time, save the Medicare trust fund a lot of money. In the past, though, even small changes to Medicare Advantage, because it is so popular, have been met with a lot of pushback from members of Congress in both parties. But that’s not really happening this time, is it?
Sanger-Katz: Yeah, This has, I think, been the biggest surprise and the most interesting part of reporting on this story. Historically, Medicare Advantage is about half of Medicare’s enrollment, as in these plans. If you survey seniors who have these plans, they tell you that they really love them. And notwithstanding all the stuff we just talked about, I think they are popular by most people who use them. In part, it’s because they get these extra benefits. They have lower premiums. You know, they get some goodies that they wouldn’t get with regular Medicare. And in Congress, the preponderance of members of Congress have signed letters indicating that they support, I think, what they call a stable policy-and-rate environment for the plan. So last year, 80% of members of the House of Representatives signed such a letter. That’s just, I mean, you don’t see 80% of members of the House of Representatives agreeing on practically anything — and a majority of senators as well. And I think everyone’s expectation, including me, is that when these people signed this letter and said, you know, this is important and my constituents care about it, that they would have the back of the plans and that it would be hard for regulators to be aggressive in trying to change anything about this program because there would be such a big political outcry. And, in fact, what’s happened is they have really started cracking down. They started with some of these smaller regulations. And then the one that they did, it was kind of hidden in a technical way, but it had a really big impact. They changed this whole formula and they basically said, hey, plans, like, you can no longer get these extra payments for a lot of the diseases that they were very commonly making money for diagnosing people for. And all of a sudden, you know, this support on the Hill just kind of dissolved. And that is very much in the face of this huge lobbying effort. You know, Julie, you mentioned the television commercials, but the plans also mobilize their customers to call their members of Congress to contact the White House. Something like 142,000 calls and letters have been submitted to members of Congress and the White House. The proposal itself, there’s the formal comment process — in a normal year [it] gets like a couple of hundred comments, mostly from various stakeholders in the Medicare system. This year there was an organized letter-writing campaign and 15,000 comments were submitted on this rate notice. So we just see this environment in which the public has been activated. Lobbyists are going crazy. The CEO of United[Healthcare], the largest health insurer in the country, was making the rounds on the Hill, talking to members of Congress. And yet … and yet there’s really no one in Congress who’s standing up and screaming and yelling about how terrible this is. I mean, I shouldn’t say no one. There are a few individual members of Congress, Republicans, who have been highly critical of this and who have pointed out that this move is potentially inconsistent with President [Joe] Biden’s promise to never cut Medicare, which is a key campaign message for him going into his reelection. But the leaders in Congress, the heads of committees, the really prominent members, and certainly leading Democrats have not said those kinds of things. There were letters that came out very late in the process, really in the last week or so, from Republicans in House and Senate committees of jurisdiction that you might have expected to be these angry, partisan, like, “how dare you do this to Medicare Advantage?” kind of letters. And they were not those kinds of letters. They weren’t critical, but they were very polite and they were very technical. They’re, like, could you please answer the following 10 very technical questions about this tiny little detail of the formula? So it’s clear … they are concerned and they are providing oversight. And I don’t think that they are enthusiastically embracing these changes. But at the same time, I think they are not carrying water for the insurance industry and making it very politically difficult for the Biden administration to make these changes.
Rovner: I feel like the Humana announcement actually sent quite a message that says, wow, we can make a lot more money from Medicare than we can make from the commercial market.
Kenen: Well, I think that’s true. I mean, one reason so many seniors are in Medicare Advantage, and do like it, is that they get an incredible deluge of marketing. I mean, the companies went in here, they saw that it was a business opportunity. They have marketed themselves very aggressively. People get dozens and dozens of letters saying, “Apply for this plan” or “We’ll give you this. We’ll give you that.” So the market is there. But I also think there’s a political dynamic that’s bubbled up recently that’s different. There’s been a fight every year about Medicare Advantage payments. It hasn’t been as grassroots; it hasn’t gotten as much attention. But there’s been a fight. I mean, every year the administration puts out their formula. Every year the industry fights it back. You know, there’s some kind of compromise. The industry doesn’t get hit as much as it would have. It’s part of the game, right? I mean, that’s how payment rules are made in Washington. But something has changed here that Biden quite successfully, at the State of the Union, really put the Republicans on the hot seat in terms of protecting Medicare and Social Security. And they’ve flipped it. Because the Republicans are better at language. You know, if this was a Republican rule, they would be calling it the “Protect America’s Seniors From Fraudulent Insurers” rule. You know … the Democrats just don’t do that.
Rovner: We should point out that it was the Republicans who named it Medicare Advantage — renamed the whole Medicare private plan program.
Kenen: Right. But just as … Biden’s politically great moment at the State of the Union making the Republicans promise not to touch Medicare, the Republicans have flipped it, because now they’re accusing Biden of attacking Medicare in a different way. And, you know, Medicare was this hot political issue in campaigns in the late Nineties and the early 2000s. It was replaced by a 10- to 15-year fight about what became the Affordable Care Act and repealing it and all that. And then there was this political vacuum in 2022, and in 2020, after the Republicans failed to repeal the ACA, we sort of had a — not health slogan-free, but it was on the back burner and …
Rovner: We had a reset. Well, we did have a pandemic.
Kenen: We had the pandemic, but — and that was politicized — but the traditional health care fight is reemerging. The traditional partisan health care fight is … both sides have accused the other over the year of “Mediscare.” This is the platform for that fight that I think we will continue to see going into 2024. I mean, it will evolve. I mean, this particular rule will get settled. But, you know, you’re sort of seeing who is the champion of Medicare, which Republicans, years ago, when Paul Ryan, when he was the budget chair of the House and the speaker of the House, he really wanted to significantly transform Medicare in ways that made it very different than the Medicare as it existed for them, Republicans, who are “saving Medicare.” For the Democrats, it was “Republicans are privatizing and destroying Medicare.” This is just Chapter 9,000. It’ll morph again between now and November 2024, but it’s begun.
Sanger-Katz: I think the politics of this are interesting and I think kind of unsettled. I’m very curious to see how this plays out in the campaigns. I do think that there is an available argument for Republicans to make that this change, which does take money out of the pockets of these plans and which potentially could mean that beneficiaries are going to end up with a little bit less generosity, because when those plans make less money, maybe they’re not going to give you as many extra goodies or lower your premium by as much. We don’t know that, but it’s certainly possible.
Rovner: In 1997, they cut payments for what was then Medicare Plus Choice, I think, Medicare Part C. And that’s exactly what happened. They cut all the extra benefits and people threw a fit, and they ended up having to put a lot of the money back.
Sanger-Katz: But in the Affordable Care Act, they cut a lot of the money and the benefits just kept growing. So we don’t know how the plans are going to absorb this change. But anyway, I think there is this available attack line for Republicans. Biden said he’s not going to cut Medicare. Look what he did. He’s cut Medicare. He’s taken all this money out of Medicare and it’s causing your premiums to go up. On the other hand, I do think there is this opportunity for Biden to say, “We reduced fraud; we improved the health of the Medicare trust fund.” And I think a lot of Republicans are actually committed to both of those things. I think they care about program integrity. They care about the fiscal future of the program. And so it’s all just a little bit scrambled. This almost feels more like something you might see in a Republican administration than a Democratic one.
Rovner: I was just saying, Jessie, is there any inclination on the Hill to do anything about this, or do you think they’re just going to either talk about it or not talk about it, as it were?
Hellmann: I haven’t heard anything about any potential action on the Hill. There’s just been letters sent asking questions, or some Republicans have sent letters saying, “We don’t like this.” But I don’t know that there’s enough support in both the Senate and the House to override this. And they are talking more about, like, the health of the Medicare trust fund. And some of the rules proposed by the administration could help strengthen that a little bit. It’s not going to solve all of its problems. But to go in and meddle with what the administration is doing to help the trust fund a little bit, while Congress is having more and more debates about helping the trust fund, I don’t know if that would be a good look.
Kenen: You could still have a policy compromise on, like, anti-fraud policy and still have a political fight. “We saved it!” “No, we saved it!” Oh, they … it’s way too soon to know what issues are going to dominate 2024 and what issues attract sustained attention from a public that doesn’t sustain attention to much of anything anymore. But right now, this is certainly a trial balloon for 2024. And I can see it. I can see that. I can see working out some kind of compromise on the actual technical issues and still having a political fight.
Rovner: Well, we’re going to move on because we’re clearly not gonna settle this today. But I hope people at least got a flavor for really how complicated this is, both, you know, technically and politically. I want to turn to something else that’s complicated: That’s reproductive health. And by that I mean much more than abortion and birth control. A new study from the Centers for Disease Control and Prevention finds that maternal mortality, the death rate for people when they are giving birth or in the weeks immediately after, rose by more than a third in 2021 compared to 2020. And African American women, even those with higher incomes, were 2½ times more likely to die during or just after childbirth than white women. Certainly, the pandemic had something to do with this. It disrupted medical care for just about everybody, and pregnant women who got covid had a higher risk of severe illness or death. But this is really just a continuation of a trend that’s been troubling health experts for several years now. Joanne, you’re our public health expert here. Why has this been so difficult to address?
Kenen: I mean, I think some of it is the two things that Julie said for 2020. I mean, you know, there was all this fear that the vaccines could hurt pregnant women. Actually, it was covid that hurt pregnant women and their babies. So, hopefully, we’re over the worst of that. And people weren’t going in for good prenatal care. So that was a factor. But this is a really sustained problem, and we’ve begun to take some steps. Most states are now extending Medicaid coverage postpartum for six months or a year under Medicaid. I think that when many of us, including me, when I first heard about these problems with maternal mortality, I was thinking about giving birth. I was thinking about hemorrhage and things that happen in the delivery room or right after, when, in fact, it’s really the full year after. There is high risk for everything. And that’s where a lot of the disparities in our system … the states that don’t have Medicaid, the states that …
Rovner: Didn’t expand Medicaid.
Kenen: … didn’t extend Medicaid, you know, or there aren’t … most of them are now expanding it for women in this category, or beginning to. So that might help. I mean, the disparities throughout the health care system, this is not just an income thing. In all economic strata, the racial disparities in maternal mortality exist. And then I just found out something recently that really shocked me. I’ve done some work over the past six months writing about domestic violence as a public health problem, and I’ve moderated two panels, just like in the last 10 days on it. And most states do not count homicide, suicide, and overdose as part of the maternal mortality figures. So if you think these figures are bad, it’s way worse, because pregnancy and postpartum are all so high risk for all of those things. But since the OB-GYNs actually review these maternal mortality cases, they’re not reviewing those other three categories. So as bad as it is, it shocked me to realize what we’re looking at and being horrified by isn’t even the full picture.
Rovner: Wow. So, well, here’s where reproductive health writ large and abortion policy cross in ways that may be unexpected to lawmakers who voted for their states’ bans, but not to anybody who’s studied health policy. In Idaho, a rural hospital has announced it will no longer deliver babies, forcing women seeking labor and delivery care to travel nearly 50 miles. Why? Because the hospital, Bonner General Health in Sandpoint, says it cannot keep enough health professionals, both OB-GYNs and pediatricians, to safely run a maternity ward. Why not? Well, Idaho’s, quote, “legal and political climate,” says the hospital from its press release, quote: “The Idaho legislature continues to introduce and pass bills that criminalize physicians for medical care nationally recognized as the standard of care.” Margot, your extra credit this week is about something similar, but in Texas. So why don’t you do it now?
Sanger-Katz: Yes, I wanted to recommend this article from Sophie Novak in Slate called “You Know What? I’m Not Doing This Anymore.” And her piece profiles a whole bunch of nurses and doctors who work in OB-GYN care in Texas who are quitting or leaving or who are considering not taking jobs that they might otherwise have taken. And I think we don’t have real data on these trends, and I’m always a little bit worried about these kinds of stories that, you know, you can always find five or six or seven or 10 doctors who are unhappy or who say that they might quit. There was a lot of those stories, like, when Obamacare passed, all these doctors are going to retire early because they don’t like the rules. I think that turned out to be more marginal than we might have expected based on that coverage. But I still think that this story is telling these stories of these providers, and I think it’s pointing to something that is a real risk and is potentially a real trend, which is if you are someone who is in the business of caring for women through pregnancy and childbirth, and you feel like you cannot do the things that you were trained to do, that there is potential criminal liability for you in providing the care that your patients need, if you’re having to watch your patients suffer through needless harm or medical risk because you can’t provide an abortion when one is medically indicated without facing that kind of legal risk. I do think that there is a real risk that these people are not going to want to practice in those states. They would rather go to a place where they have a little bit more autonomy and a little bit less concern about prosecution. And what that means is that the women left behind in these states, however you feel about abortion, may not have access to as many health care providers, and they are going to continue to have pregnancies and births and need that kind of support. And I think that is a very interesting and troubling dynamic that I think could have very large reverberations and could, of course, make the trends that Joanne was just talking about, you know, even more concerning and lead to even more disparities. Because, of course, it is a lot of the states that are banning abortion are states that have these kind of poor, minority communities who are already facing a lot of the maternal mortality. We see in the existing data it’s increasing in a kind of across-the-board way, but there are some places where it’s worse than other places. And a lot of the worst places for maternal and fetal mortality are these same places that are banning abortion and where they may be at risk of losing some of the providers that can help ameliorate the problem.
Rovner: And it’s not just losing the providers, it’s replacing the providers who do get old enough and retire or who leave, because we’re seeing medical students, fourth-year medical students, say they’re loath to apply for residencies in some of these states, partly because they’re worried about their training, but partly because, you know, if they’re women, they may need this care at some point or they may have family members who will come with them who need this care at some point. And because, for the most part, where you do your residency tends to be where you end up practicing. So, I mean, we didn’t see it so much in this year’s match, but I’m wondering whether this is going to be an issue, too. There’s some big, important academic training centers in some of these states with bans. I’m thinking, you know, Vanderbilt comes to mind immediately in Tennessee. I think this is another thing that was perhaps unexpected, although if you thought about it hard, you could have predicted it.
Kenen: I mean, pregnancy is complicated. A century ago, women commonly died in pregnancy. And we live in an era where it’s safer than it had been, but we forget it can still be risky. And wanted pregnancies, very much wanted pregnancies, can go wrong. And I’ve experienced … I mean, I have two kids, but I experienced that, and I needed emergency medical care and I was able to get it. I needed emergency medical care more than once, and I was able to get it.
Rovner: And I remember visiting you when you were on bed rest.
Kenen: Right? It was one of my few fun nights on bed rest, when Julie and Joanne Silberner brought me dinner. We had a picnic, right? In bed, right? But, you know, I never had to deal with anything except the grief of losing a pregnancy. So, you know, it was a very much wanted pregnancy, and I didn’t have to worry about anything being withheld from me. I had a lot of things go wrong a lot of times. But, you know, I was really lucky to end up with the family I have. When I read these stories, and I go back and think, what if I had to deal with infection? What if I couldn’t get that care? And we’re just not thinking this assumption, by mostly male lawmakers, that it’s not a huge medical thing. Pregnancy changes your body, everything about your body, it’s not just cosmetic. There are lots and lots of risk factors, before and after. That [has] sort of just been glossed over as, oh, it’s not a problem. And it is a problem. And one reason we’re going to see this shift in medical practice is because they understand it’s a problem. I mean, you read these stories about these doctors, and we’ve talked about them every week, and our listeners have heard them and read them, about doctors who are watching a patient with a serious infection, until she is getting close enough to die that they can treat her, but not so close to dying that they lose her. And you hear the anguish.
Rovner: That’s why I was so taken by that line in the press release from the hospital in Idaho, which is that doctors don’t want to possibly be criminalized for what is considered the standard of care. They’re being asked to basically choose between perhaps getting sued or put in jail and what they vowed to do to care for their patients. And it’s really hard. It’s not really that much of a surprise that people are going to leave or not go there. All right. Well, we will definitely come back to this, too. I want to talk about covid briefly. Jessie, the president signed the bill passed by Congress to declassify intelligence on the origin of covid. Do we have any idea when that’s going to happen? How soon? And do we get to see this, too? Or just the members of Congress?
Hellmann: The director of national intelligence is supposed to declassify this information 90 days after the law is passed. After that, I’m not entirely sure if it’s just for Congress or it’s for the public, to be honest.
Rovner: We will see. I was amused that, right after this happened — because now we have all this talk that, you know, “Oh, absolutely” or not, absolutely it was a lab leak, but “more likely it was a lab leak.” Now we have new evidence suggesting that it may, in fact, have started in the Wuhan wet market, after all, jumping from something called raccoon dogs? Now, I consider myself something of an animal expert here. I have never heard of a raccoon dog.
Sanger-Katz: They’re really cute. I was enjoying looking at all the photographs of them.
Rovner: Are we going to now go back to the “OK, maybe it really did come from the market”? I-I-I …
Kenen: What I’m about to say is an oversimplification, but if you’re a Republican, you think it’s a lab leak. And if you’re a Democrat, you think it’s a raccoon dog. And that is an oversimplification. And one of the things that drives me crazy is that the potential for lab leaks exists and lab safety is an issue that should be bipartisan. There have been lab leaks in the U.S., there have been lab leaks elsewhere in the world. And that doesn’t mean this came from a lab leak, but lab leaks are a thing. And we want to make them not a thing. But again, there are many lessons we should be able to take from the pandemic; that’s one of them. Like, OK, maybe this wasn’t a lab leak, maybe this was the Wuhan animal market, but let’s take this as a moment to think about how we can protect ourselves from a future lab leak. You know, we may never conclusively know. Even the raccoon dog thing is still a theory. I mean, there’s evidence behind that theory, but the scientific establishment has not said, OK, this is it. There’s still debate. The science world tends to think it’s zoonotic, that it’s from an animal, but it’s not over yet. And again, the politicization is preventing good public policy.
Rovner: If only someone could turn that fight into something. And as I quoted Michael Osterholm last week as saying, “It doesn’t matter which one it was, because we have to be ready for both of them in a future pandemic.”
Kenen: Exactly. And we’ll probably have both. I mean, we may not have a pandemic from a lab leak, but is it possible that somebody, somewhere, or some community will be hurt from a lab leak? Yes, it is. And we need to mitigate that. Is it possible we have another zoonotic infection? I mean, there’s two Marburg outbreaks in Africa right now. I mean, that’s from animals. And there’s two of them going on. It’s an obscure disease. It’s worse than Ebola. It doesn’t spread as fast, but we have zoonotic infections way more often than the average American realizes.
Sanger-Katz: And also just one more thing, which is we still had and have a global pandemic that has caused enormous suffering and death and fear around the world. And in some ways, I feel like this obsession with like whose fault it is is a distraction from what can we do to prevent such a thing from happening in the future and really looking at, like, what was done appropriately and inappropriately in terms of the covid response? Pinning this down seems … it seems academically interesting to me. It seems useful to know. I think, as you guys have said, you’ve got to be ready for both things anyway. But it also feels like a little bit of a sideshow sometimes when the reality is: Covid came for us. It wasn’t a near-miss where looking at the origin is the whole story. It’s also everything that came afterwards is really important, too.
Rovner: Yes, absolutely. Well, finally this week, one more update. On last week’s podcast,while we were discussing Novo Nordisk following Eli Lilly’s lead in announcing insulin price cuts, I wondered aloud how long it would be before the third company in the triumvirate that controls most of the diabetes drug market, Sanofi, would follow suit. As it turned out, the answer was a couple of hours. In a press release that came out Thursday afternoon, Sanofi said it would cut the price of its most popular insulin product by 78% and ensure that people with health insurance pay no more than $35 a month for their insulin. But I’m thinking this fight is not completely over; now that the three big companies have voluntarily said we’ll lower our prices on some of our insulins, Congress is still going to want to do something about this, right?
Hellmann: Yeah. Sen. [Chuck] Schumer said last week that he still wants Congress to address this issue. He still wants to cap the cost of insulin because, like you said, there are still insulin products that some of these companies offer that don’t fall under these announcements.
Rovner: Drug prices will continue to be a top-of-mind issue, I suspect. All right. Well, that’s as much news as we have time for this week. Now it is time for our extra-credit segment. That’s when we each recommend a story we read this week we think you should read, too. As always, don’t worry if you miss it. We will post the links on the podcast page at kffhealthnews.org and in our show notes on your phone or other mobile device. Margot, you’ve already done yours. Joanne, why don’t you go next?
Kenen: It’s a piece in The New Yorker, and I’m not sure how she pronounces her name. I think it’s Jia Tolentino. If any of you know, please correct me. But the story is called “Will the Ozempic Era Change How We Think About Being Fat and Being Thin?” I mean, this is a diabetes drug that is being used off-label for weight loss, quite widely to the point that there’s a shortage for people who have diabetes; they are having trouble getting it. It does help people lose weight and it’s become very much in demand because it does help you lose weight. And there are a few others in this class. So, the question she poses: This is a metabolic disorder, it’s not just a willpower issue, and will this help us get to that point? … It was a really good, interesting article, and I still ended up with a lot of questions about long-term safety, about do you have to take it forever and how much, and what happens if you don’t? It’s treating obesity rather than thinking about how to prevent obesity, which is a better — you know, too late for some millions of Americans, but there is generations to come. So but it was an interesting, provocative landscape piece.
Hellmann: My story is from The Washington Post. It’s called “Senior Care Is Crushingly Expensive. Boomers Aren’t Ready.” It’s just a story about how expensive long-term care could be, especially if you need really specialized care. One of the people interviewed for this story would have to pay about $72,000 a year to stay in an assisted-living facility. This person has Alzheimer’s and so they just need a little more help than someone else might. And they talk a lot about how Medicaid will cover some of this care, but only if you spend all of your life savings. And obviously, Medicare doesn’t really cover stays in assisted-living facilities either. I know we talked in email about how perennial this issue is. It’s something that was an issue 20 years ago. People are warning: We need to fix this problem.
Rovner: More than that. When I first joined CQ in 1986, it was the first big story I wrote, about what are we going to do about long-term care for the baby boomers? Here we are almost 40 years later, still talking about the same thing.
Hellmann: Yeah, I guess the answer is nothing.
Rovner: Not much has happened.
Kenen: Yeah, what’s happened is we’ve shifted more and more of it onto families.
Rovner: Yeah, that’s true.
Kenen: More complicated care for longer.
Rovner: My extra credit this week is a truly terrifying piece from Vice News called “Inside the Private Group Where Parents Give Ivermectin to Kids With Autism,” by David Gilbert. And the headline says most of it. What it doesn’t say is that when you give horse wormer to kids — and this group actually advises the use of the paste that’s given to horses — they’re going to have adverse reactions. The kids, not the horses, including headaches, stomachaches, blurry vision, and more. But the administrators of this group insist that the side effects aren’t because the children are being administered something that can kill people in the wrong dosages, but because the medication is, quote, “working.” They also say it can cure a whole host of other disorders from Down syndrome to alopecia. It is quite the story. You really do need to read it.
OK. That is our show for this week. As always, if you enjoy the podcast, you can subscribe wherever you get your podcasts. We’d appreciate it if you left us a review — that helps other people find us, too. Special thanks, as always to our ever-patient producer, Francis Ying. As always, you can email us your comments or questions. We’re at whatthehealth — all one word — at kff.org. Or you can tweet me. I am @jrovner. Margot?
Sanger-Katz: @sangerkatz
Rovner: Jessie.
Hellmann: @jessiehellmann
Rovner: Joanne.
Kenen: @JoanneKenen
Rovner: We will be back in your feed next week. Until then, be healthy.
Credits
To hear all our podcasts, click here.
And subscribe to KHN’s What the Health? on Spotify, Apple Podcasts, Stitcher, Pocket Casts, or wherever you listen to podcasts.