What You Need to Know About the Opioid Settlement Funds
States and localities are receiving more than $54 billion over nearly two decades.
Se hacen públicos por primera vez los pagos a los gobiernos locales por el acuerdo sobre opioides
Algunos estados, como Carolina del Norte y Colorado, han publicado en internet los detalles de su distribución. Pero en la mayoría de los lugares es complicado.
Opioid Settlement Payouts to Localities Made Public for First Time
KFF Health News obtained documents showing the exact dollar amounts — down to the cent — that local governments have been allocated in 2022 and 2023 to battle the ongoing opioid crisis.
Find Out How Much Opioid Settlement Cash Your Locality Received
You can use documents obtained by KFF Health News to see the exact dollar amounts that local governments in your state have been allocated in 2022 and 2023.
International Rights Group Calls Out US for Allowing Hospitals to Push Millions Into Debt
In a new report, Human Rights Watch urges stronger federal and state action to hold hospitals to account for a medical debt crisis that now burdens more than 100 million Americans.
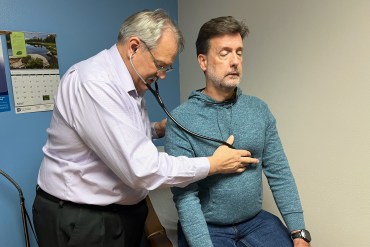
Burnout Threatens Primary Care Workforce and Doctors’ Mental Health
Burnout is a widespread problem in the health care industry. Although the pandemic made things worse, burnout among doctors is a long-standing concern that health systems have become more focused on as they try to stop doctors from quitting or retiring early.
As Fewer MDs Practice Rural Primary Care, a Different Type of Doctor Helps Take Up the Slack
The number of DOs is surging, and more than half of them practice in primary care, including in rural areas hit hard by doctor shortages.
Watch: Payback for the Opioid Crisis: How Did the Sackler Family Skirt Liability?
KFF Health News senior correspondent Aneri Pattani appeared on PBS NewsHour to discuss the ruling surrounding drugmaker Purdue Pharma’s role in the opioid crisis and her reporting into the ongoing distribution of opioid settlement funds.
Medicaid: más de medio millón ya han perdido cobertura desde fin de beneficios pandémicos
Hasta ahora, 4 de cada cinco personas que perdieron la cobertura nunca devolvieron la documentación requerida, según un análisis de datos de 11 estados.
As Medicaid Purge Begins, ‘Staggering Numbers’ of Americans Lose Coverage
In what’s known as the Medicaid “unwinding,” states are combing through rolls to decide who stays and who goes. But the overwhelming majority of people who have lost coverage so far were dropped because of technicalities, not because officials determined they are no longer eligible.
Many People Living in the ‘Diabetes Belt’ Are Plagued With Medical Debt
The “Diabetes Belt,” as defined by the Centers for Disease Control and Prevention, comprises 644 mostly Southern counties where diabetes rates are high. Of those counties, KFF Health News and NPR found, more than half also have high levels of medical debt.
He Returned to the US for His Daughter’s Wedding. He Left With a $42,000 Hospital Bill.
After emergency surgery, an American expatriate with Swiss insurance now carries the baggage of a five-figure bill. Costs for medical care in the U.S. can be two to three times the rates in other developed countries, so foreigners and expats with good insurance in their home countries need travel insurance to protect themselves from “crazy prices.”
A Rural County’s Choice: Use Opioid Funds to Pay Off Debt, or Pay Them Forward to Curb Crisis
Greene County, Tennessee, so far has received more than $2.7 million from regional and national settlements with opioid manufacturers and distributors. But most of the money is not going to help people and families harmed by addiction.
Biden Administration Issues New Warning About Medical Credit Cards
Americans paid an estimated $1 billion in deferred interest on medical debt in just three years, the Consumer Financial Protection Bureau reports. The agency warns against medical credit cards, which are often pitched right in doctors’ offices.
Community Paramedics Don’t Wait for an Emergency to Visit Rural Patients at Home
Community paramedicine is expanding nationwide, including in rural areas, as health care providers, insurers, and state governments recognize its potential to improve health and save money.
After Idaho’s Strict Abortion Ban, OB-GYNs Stage a Quick Exodus
At least two Idaho hospitals are ending labor and delivery services, with one citing the state’s “legal and political climate” and noting that “recruiting replacements will be extraordinarily difficult” as doctors leave.
Listen: How Are States Spending Money From the Opioid Settlements? It’s Not Easy to Know
KFF Health News senior correspondent Aneri Pattani appeared on NPR’s “1A” on May 1 to discuss issues related to how opioid settlement funds are being distributed.
Expectant Mom Needed $15,000 Overnight to Save Her Twins
Doctors rushed a pregnant woman to a surgeon who charged thousands upfront just to see her. The case reveals a gap in medical billing protections for those with rare, specialized conditions.
A California Physician Training Program Adds Diversity, but Where Do Graduates End Up?
Researchers found that, while a University of California medical training program has diversified the system’s pool of medical students, there’s not enough long-term data to know whether graduates return to practice where they’re needed most.
The Biden Administration Vowed to Be a Leading Voice on Opioid Settlements But Has Gone Quiet
Billions of dollars are headed to state and local governments to address the opioid crisis. Policy experts and advocates expect the federal government to play a role in overseeing the use of the money. Failure to do so, they say, could lead to wasted opportunities. And, since Medicaid helps pay health care costs, the feds could have a claim to portions of states’ opioid settlements.